Patent foramen ovale (PFO) is common and occurs in 20–34% of the population.1 In most infants, the foramen ovale closes soon after birth, with a reduction in pulmonary vascular resistance raising the left atrial pressure above that of the right atrium during the first few breaths, closing the septum. In a significant proportion of individuals, the primum and secundum atrial septa do not fuse, and the foramen ovale remains incompletely closed. There is a residual, but transitory, communication between the right and left atria, particularly likely to open during actions that cause sudden rises and falls in intrathoracic pressure, such as sneezing, coughing or straining. The pressure changes that transiently open a PFO can often be produced by asking patients with a PFO to perform and then release a Valsalva manoeuvre.
In most adults, a PFO will appear only as a chance finding during cardiac investigation, or more likely remain undetected. Some PFOs may open widely, providing a conduit for thrombus, air or vasoactive peptides to travel from the venous to arterial circulation – causing a paradoxical embolus. This transfer is associated with several clinical phenomena, including cryptogenic stroke, systemic embolus, migraine with aura and decompression sickness in divers. Percutaneous PFO closure provides a practical and elegant solution to the problem of PFO in carefully selected individuals. This review evaluates the evidence for PFO closure, discusses which patients should be considered for this treatment and reviews how the procedure should be undertaken.
The Anatomy of a Patent Foramen Ovale
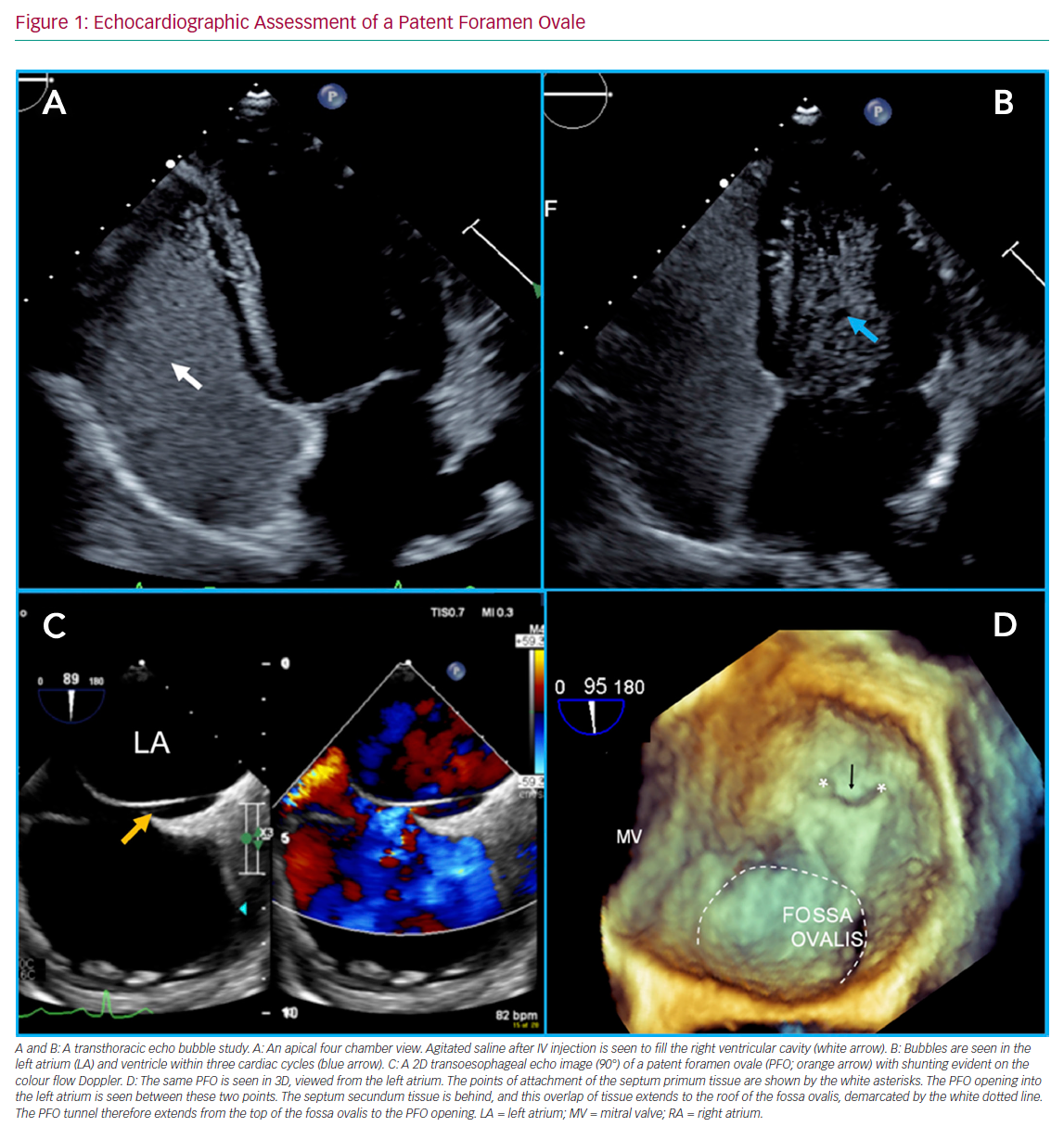
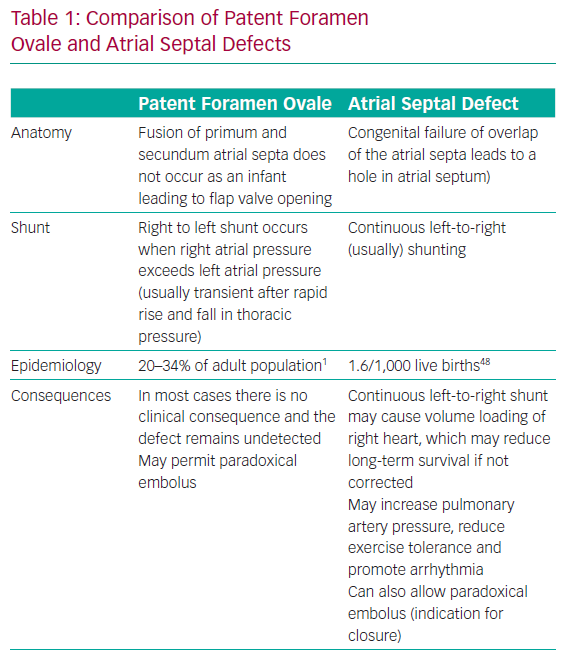
As the heart develops in the foetus, the primum and secundum septa grow and overlap. At birth, the PFO should close. In patients with a PFO, the atrial septal growth is normal; however, the communication between the right and left atria (PFO) fails to close postpartum (Figure 1). This phenomenon is distinct from a hole in either septum, which would constitute an atrial septal defect (ASD) – a separate entity with different functional consequences and different indications for closure. Table 1 compares PFO and ASD.
Despite their differences, both PFOs and ASDs may permit the transit of a paradoxical embolism. The overlapping of the primum and secundum atrial septa in a PFO forms a flap valve that usually only opens when the right atrial pressure exceeds the left atrial pressure. PFOs are functionally closed most of the time, as right atrial pressure is usually less than the left atrial pressure. This pressure gradient can be reversed by manoeuvres that change the intrathoracic pressure (e.g. sneezing, coughing or straining to defecate), allowing the PFO to open, and blood, thrombus or any other substance to pass across from the right to left atrium.
Indications for Patent Foramen Ovale Closure in 2019
Cryptogenic Stroke
Often, despite extensive investigation, a clear cause cannot be found for stroke. Causes that can be identified include AF, atherosclerotic disease, carotid dissection and intracerebral pathology, such as haemorrhage or space-occupying lesions.2,3 The cause of stroke remains unknown in up to 40% of patients with a stroke diagnosis. These are designated as cryptogenic stroke. In the presence of a PFO, the presumed cause of stroke is paradoxical embolus. As the likely cause is known, the term ‘cryptogenic’ is a misclassification, but remains in use throughout the literature. An alternative term is embolic stroke of undetermined source, which was first used in 2014. This still misclassifies stroke from paradoxical embolism, where the cause is known.4–6
Zahn first described paradoxical embolus in 1881.7 Translocation of venous thrombus to the arterial circulation under the haemodynamic conditions in which a PFO is open leads to embolic stroke. Transit of thrombus occurs after a rapid rise and fall in right atrial pressure through the aforementioned mechanisms. The PFO channel briefly provides a communication between the atria. This mechanism is supported by case studies showing thrombus across a PFO.8–10 There is also an association between cryptogenic stroke and venous thrombosis in patients with a PFO.11
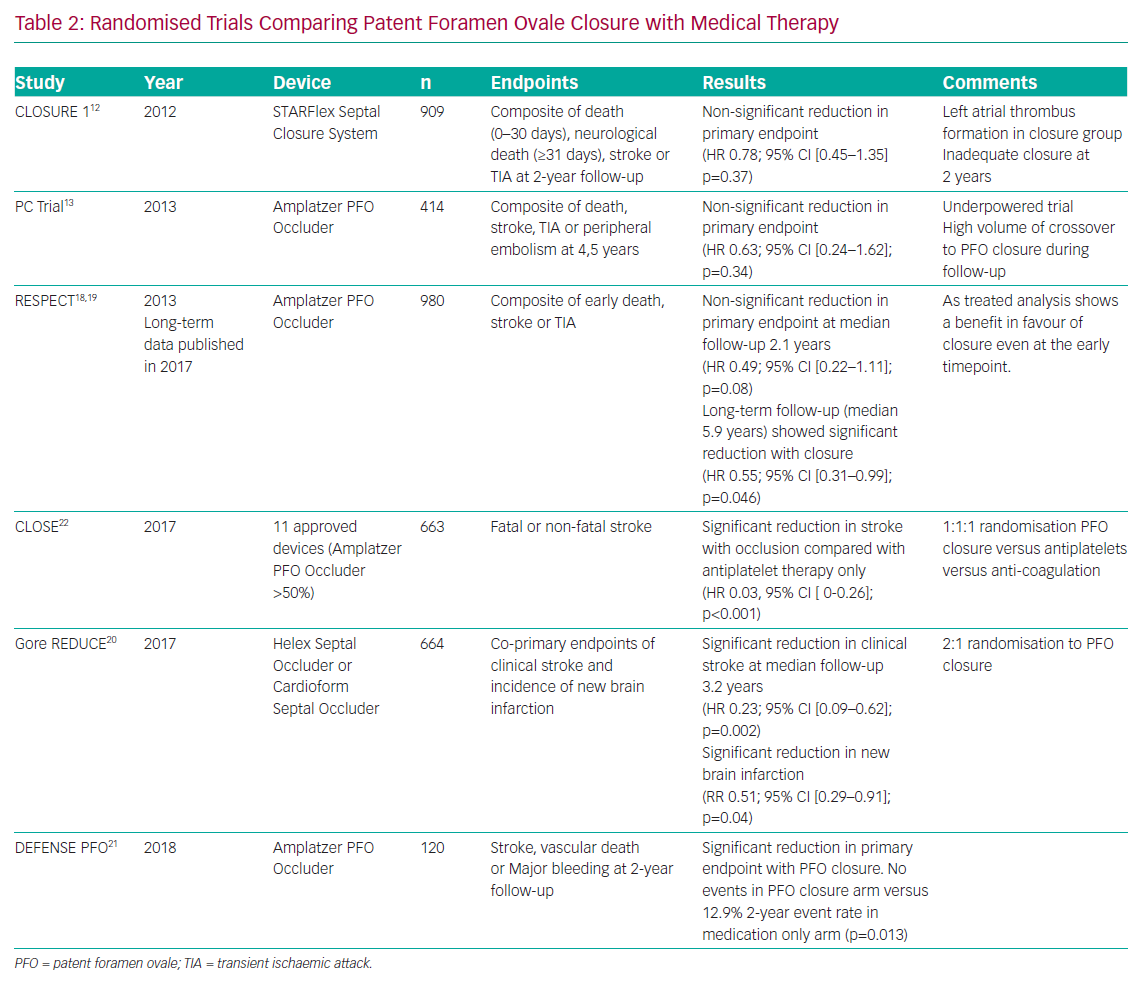
The earliest randomised trials of PFO closure (Evaluation of the STARFlex Closure System in Patients with a Stroke and/or Transient Ischemic Attack due to Presumed Paradoxical Embolism Through a Patent Foramen Ovale [CLOSURE I] and Percutaneous Closure of Patent Foramen Ovale Using the Amplatzer PFO Occluder With Medical Treatment in Patients With Cryptogenic Embolism [PC Trial]) did not demonstrate the superiority of closure compared with medical therapy.12,13 However, the studies were confounded by limited power, high crossover between groups, failure to randomise those patients whose strokes were likely to have been caused by PFO and inconsistent use of anticoagulants in the medical therapy group.14 In addition, the STARFlex occluder used in CLOSURE I has been abandoned in Europe due to concerns around residual defects and left-sided thrombus formation.15 Some have concluded that numerical equipoise in these trials were enough to recommend a one-off mechanical vaccination paradoxical embolus rather than lifelong anticoagulation.16,17 However, PFO closure was given a Class III recommendation in the 2014 American Heart Association/American Stroke Association guidelines based on the results of these trials.
Nonetheless, further randomised trials learned lessons from earlier neutral studies and have demonstrated that PFO closure is superior to medical therapy for the prevention of recurrent stroke. Early results from the Randomized Evaluation of Recurrent Stroke Comparing PFO Closure to Established Current Standard of Care Treatment (RESPECT) trial were neutral for PFO closure but extended follow up of patients demonstrated a reduction in ischaemic stroke compared to medical therapy (HR 0.55; 95% CI [0.31–0.999]; p=0.046; number needed to treat [NNT] 45).18,19 The Gore Septal Occluder Device for PFO Closure in Stroke Patients (REDUCE) clinical study demonstrated that PFO closure produced significant improvement in the clinical ischaemic stroke rate (1.4 versus 5.5%; p=0.002; NNT=25) compared with antiplatelet therapy alone.20 The Device Closure Versus Medical Therapy for Cryptogenic Stroke Patients With High-Risk PFO (DEFENSE PFO) study showed that PFO closure reduced a composite endpoint of stroke, vascular death and thrombolysis in MI major bleeding at 2 years compared with medical therapy (0 versus 12.9%; p=0.013; NNT=8).21 Finally, in the PFO Closure or Anticoagulants Versus Antiplatelet Therapy to Prevent Stroke Recurrence (CLOSE) trial, no patient receiving PFO closure experienced an ischaemic stroke compared with 14 in the antiplatelet group (HR 0.03; 95% CI [0–0.26]; p<0.001; NNT=17).22
Meta-analyses of these trials confirm that PFO closure reduces the risk of ischaemic stroke in patients with a PFO and cryptogenic stroke.23-25 Absolute risk reduction is low (1.0 stroke per 100 patient-years), but this needs to be weighed against the prolonged period that younger patients are likely to be at risk. Patients with atrial septal aneurysm or large shunts may obtain greater benefit. In these trials, and in subsequent meta-analyses, AF occurred more frequently in patients who underwent PFO closure than those receiving medical therapy alone. However, this finding did not seem to counteract the overall stroke reduction in this population. Randomised trials of PFO closure for the prevention of recurrent ischaemic stroke are shown in Table 2.
Observational data suggest that post-closure AF may be transient, with a lower stroke risk than AF with other aetiology.26 No trial or observational study has demonstrated a reduction in mortality with PFO closure, and indeed meta-analysis of multiple trials has not found a significant effect either.27–29 There may be a benefit, but it will remain difficult to prove without large randomised trials with very long follow-up periods.
Patients enrolled in PFO closure trials were young, with few studies enrolling patients age >60 years. Older patients may have an increased absolute risk of paradoxical embolus, but untangling this from other causes of stroke that also increase over time is challenging. Patients needed to have symptoms consistent with stroke and confirmation of ischaemia or infarction on cross-sectional brain imaging. Transoesophageal echocardiographic confirmation of the presence of a PFO was also required. Studies excluded patients with an alternative attributable cause for their stroke, and required enrolment no longer than 6–9 months after the index stroke.
One of the major alternative explanations for embolic stroke is AF, and this was excluded in all patients. Studies have demonstrated that over the medium to long term, PFO closure is cost-effective in both the US and UK healthcare systems.30–32 Furthermore, longer-term observational studies have shown very low stroke rates (<1%), even up to 12 years after PFO closure.33
The strict criteria of these studies are important and should be respected in clinical practice. There is little or no evidence for treatment of PFO outside these criteria, and there is no symptomatic benefit to closure in patients with cryptogenic stroke. Patients who meet trial criteria for closure should be considered for this treatment in preference to medical therapy. Patient selection is best decided in a multidisciplinary team meeting including neurology/stroke physicians, and implanting and imaging cardiologists.
Systemic Embolisation
Paradoxical emboli are likely to present with ischaemic stroke, as the brain is exquisitely sensitive to ischaemia and also receives a large proportion of cardiac output. However, systemic embolisation to the limbs, gut and down the coronary arteries have been described.10,34–36 No randomised trial evidence exists to show that closure of PFO in the case of otherwise unexplained systemic embolisation is protective. However, closure would seem to be a reasonable strategy in select cases. For example, closure of PFO would be indicated in a young patient presenting with acute MI of embolic source, with otherwise unremarkable coronary arteries and an absence of risk factors for atherosclerosis or atrial fibrillation. The indications are similar to those for cryptogenic stroke. Importantly, care must be taken to exclude alternative causes, and this may require intravascular imaging, such as optical coherence tomography, to exclude plaque rupture in the coronary artery. Cardiac MRI is also recommended to confirm a pattern consistent with MI.
Decompression Illness
Divers and high-altitude pilots, who rapidly transition from high- to low-pressure environments, may suffer from decompression illness. Sudden changes in pressure causes nitrogen bubbles to form within tissues and accumulate in the venous circulation. These bubbles are filtered from the bloodstream through pulmonary capillary diffusion, but if a return to low pressure (or ascent from depth for divers) is too rapid, then this pulmonary filtration process can be overwhelmed. Gas bubbles can enter the systemic arterial circulation.37 Bubbles continue to enlarge, causing tissue trauma and even vessel occlusion. There is a wide range of symptoms, from mild muscle and joint pain, dizziness, fatigue, headache, rash and paraesthesia, to severe breathing difficulties, confusion, motor incoordination and paralysis. A right-to-left shunt, such as a PFO, allows nitrogen bubbles to bypass the pulmonary filter, increasing the risk that usually safe ascents will cause systemic embolisation.
Diving profiles are usually designed to limit the time at depth, and slowly ascend towards the surface, minimising the risk of decompression illness. Occurence of decompression illines, despite use of safe dive profiles, implies an increased risk of right-to-left shunt. Investigation for atrial septal defect or PFO should be considered.38,39 A longitudinal, non-randomised follow-up study showed that PFO closure reduced both symptomatic neurological events and total brain lesions among recreational divers with PFO and decompression illness, compared with those who continued to dive without closure.40
A recent prospective registry evaluated 489 recreational divers for PFO using transcranial Doppler. This demonstrated that large PFO was a major independent risk factor for unprovoked decompression illness (HR 92; 95% CI [12.5-689]; p<0.001).41 A recent study noted that in a cohort of 59 divers with decompression illness and PFO closure, four continued to have decompression illness over the 10-year follow-up period. This was shown to be due to residual shunting, despite reported successful closure.42 Where a professional diver wishes to continue diving, PFO closure could be recommended. Alternatively, discontinuation of diving or curtailing provocative dive profiles should be considered. If diving is recreational, then the risk–benefit analysis for continued diving with a PFO closure is less clear, and certainly procedural risk should be carefully weighed against the benefits of continuing to dive.
Platypnoea–Orthodeoxia Syndrome
Platypnoea–orthodeoxia syndrome is a rare condition characterised by dyspnoea and positional desaturation in individuals with a PFO. In certain body positions, the geometry of the atrial septum is altered, allowing a continuous stream of deoxygenated blood from the inferior vena cava to flow across the PFO. Deoxygenation is typically seen when the patient is seated, but oxygen saturations normalise when the patient lies flat.43 The distortion of the atrial septal geometry can be caused by thoracic and cardiothoracic surgery, such as pneumonectomy, aortic dilatation and aortic surgery, or may not have an identifiable cause.
Regurgitant jets from the tricuspid valve can also be directed across the PFO. Underlying cavity pressures do not affect platypnoea–orthodeoxia syndrome, and it responds well to PFO closure so long as pulmonary artery pressures are not markedly elevated. This is not usually the case. A 54-patient case series demonstrated that percutaneous closure was safe and effective for platypnoea–orthodeoxia syndrome.44
Migraine with Aura
Migraine is common in young people. It is associated with aura in approximately one-third of cases.45,46 Migraine with aura has been associated with right-to-left shunts, such as PFO.47,48 Large shunts are particularly associated with migraine with aura.49 Transfer of a vasoactive substance, usually filtered by the pulmonary circulation into the systemic circulation, is the proposed mechanism for the relationship between migraine and PFO.47
A number of non-randomised studies reported improvement in patient symptoms after closure.50 In the Migraine Intervention With STARFlex Technology (MIST) trial, patients with refractory migraine with aura were randomised to either percutaneous PFO closure or a sham procedure. There was no difference in cessation of headache or reduction in headache-free days. However, the trial population had a relatively low frequency of migraine, and a high frequency of residual shunts after closure – this trial used the same prosthesis as the negative CLOSURE 1 stroke trial with similar issues. These confounders may have negatively influenced the trial result.51
More recently, the Percutaneous Closure of PFO in Migraine with Aura (PRIMA) and Prospective Randomised Investigation to Evaluate Incidence of Headache Reduction in Subjects With Migraine and PFO Using the Amplatzer PFO Occluder Compared With Medical Management (PREMIUM) trials have reported their results.52,53 Both studies were negative for their primary endpoints, although there were some reductions in headache. These effects were small and occurred at the expense of procedural complications. The evidence for PFO closure is not strong enough to offer a routine recommendation for PFO closure in migraine with aura.
The Patent Foramen Ovale Closure Procedure
Pre-procedure Investigations
As cryptogenic stroke is the most common indication for closure, an emphasis should be placed on investigation looking for alternative causes of stroke. Cross-sectional brain imaging should be undertaken to confirm the diagnosis of an embolic stroke. Lacunar strokes are unlikely to be embolic in nature.
AF is the most common source of thrombus, with studies suggesting that 13% of patients with AF have cardiac thrombus.54 In 90% of patients with non-valvular AF, the thrombus was located in the left atrial appendage.54 The presence of AF in the context of a stroke is an indication for anticoagulation, and closure of a PFO is not indicated.
No study has shown that closure of a PFO confers additional benefit. ECG monitoring is mandatory to exclude AF, and the duration depends upon the patient’s risk factors. We recommend in young patients (<50 years) with no risk factors, using a minimum of 72-hour ambulatory surface electrocardiographic recording, and in those aged >50 years, using 6 months of implantable loop recording. Implantable loop recording has the advantage of extended rhythm surveillance; however, it is prone to false positives and false negatives.55–57 Conclusive evidence for the best strategy to diagnose AF is lacking. The high burden of supraventricular ectopics on ambulatory ECG or enlarged atrial size increases the likelihood of AF, and may indicate that an implantable loop recording is required in a younger patient.
Carotid imaging should exclude significant carotid plaque disease. Screening for thrombophilia should be considered, but its complex nature with inconsistent results means repeated investigations are often required. Thrombophilia often predisposes to venous rather than arterial thrombosis. Interpretation of complex results can be difficult, and should be undertaken in conjunction with haematologists who have a special interest in thrombosis.
The first-line investigation to exclude intracardiac thrombus is transthoracic echocardiography. A number of conditions, apart from AF, are associated with cardiac thrombus, which could embolise to cause stroke. These include MI, left ventricular aneurysm, atrial myxoma, non-compaction cardiomyopathy, left ventricular failure and mitral stenosis. Prior to closure of PFO, these should all have been excluded as the potential source of the stroke.
A key investigation while working up patients with cryptogenic stroke is bubble contrast echocardiography. A PFO needs to produce a right-to-left shunt to cause a stroke. Bubble contrast studies are initially performed with transthoracic echocardiography, with no sedation necessary. Agitated saline is injected via a peripheral venous cannula (ideally placed in the lower body, but the left antecubital fossa is usually a more realistic option), while the patient releases a Valsalva manoeuvre or sniff. In the presence of a cardiac shunt, bubbles should appear in the left side of the heart within three to four cardiac cycles of arrival in the right atrium. Later appearance of bubbles may reflect a pulmonary shunt. The study should be performed by an experienced operator. The procedure may require multiple repeats to confirm the diagnosis. Figure 1 shows a bubble study with transmission of bubbles from right-to-left. Transcranial Doppler is a non-invasive alternative to a contrast echocardiogram. It is a reliable method of assessing for the presence of a right-to-left shunt, although it does not delineate the anatomy of the PFO.58,59
A positive transthoracic bubble study or transcranial Doppler study after a cryptogenic stroke indicates the need for detailed transoesophageal echocardiography (TOE). A further bubble study can be undertaken using TOE if required. This allows the structural heart team to accurately determine the anatomy of the PFO. Assessment of a PFO is shown in Figure 1. A TOE also allows the exclusion of alternative shunts, such as ventricular septal defects, anomalous pulmonary venous drainage or sinus venosus defects. A detailed guide to TOE assessment of PFO is outside the scope of this review, and is well reviewed elsewhere.60
Multiple specialties (including stroke physicians or neurologists, cardiac imaging specialists, radiologists and interventional cardiologists) are involved in diagnosis and treatment decisions for cryptogenic stroke with PFO. Investigation should be considered in a multidisciplinary setting, with a holistic approach to the management of the patient.
The Closure Procedure
Closure is performed as a day case procedure in many centres. The procedure can be undertaken in a standard catheter laboratory using fluoroscopic guidance and physiological monitoring. Patients undergoing this procedure will have a reduced long-term risk of stroke, but obtain no immediate symptomatic benefit from this procedure. Therefore, all possible steps to reduce complications should be taken.
In the opinion of the authors, the procedure should be, as far as possible, complication-free, because even a small complication rate is likely to neutralise the benefit over optimal medical therapy. Ultrasound-guided femoral venous access, echocardiographic guidance, adequate anticoagulation and special care to reduce the risk of air embolus are all important to ensure this goal.
Periprocedural guidance with TOE or intracardiac echocardiography is mandatory, in the opinion of the authors, to consistently achieve the best result.61,62 Furthermore, it is considered mandatory within commissioning guidelines in the UK, and recommended in the Society for Cardiovascular Angiography and Interventions 2019 consensus statement.63,64
Although the procedure can be undertaken by very experienced operators with fluoroscopy alone, echocardiographic guidance allows evaluation of interatrial septal anatomy, direct visualisation of the device position, and the relationship with aortic and mitral valves before device release. General anaesthesia is generally required to facilitate TOE, which may increase the cost and length of the procedure.
The procedure is undertaken from the femoral vein with ultrasound guidance for the puncture. Adequate anticoagulation (unfractionated heparin 80–100 IU/kg) should be administered. A 6-Fr multipurpose diagnostic catheter and a 0.035" J-tipped guidewire is used to cross the PFO and is passed into a pulmonary vein (usually the left upper pulmonary vein). This can then be exchanged for a stiff wire to assist delivery of balloons.
Sizing of the PFO can be undertaken both before and after crossing with the wire, which may result in the PFO tunnel widening and shortening. Three-dimensional imaging software can be used to determine the maximum left and right atrial opening and minimum tunnel length. Balloon sizing of the PFO is usually not required, but can be performed using quantitative angiographic tools, and confirmed with TOE or intracardiac echocardiography. A left anterior oblique cranial fluoroscopic projection may assist with this, as the septum is seen in profile. Compliant balloons with marked graduations are used, but balloon sizing can still shorten and widen the PFO. Shortening may be desirable if there is a particularly long PFO tunnel, but this can increase the size of the hole, necessitating a larger device. Factors that predispose to a larger device include PFO tunnel length, the presence of atrial septal aneurysm and male sex.65 Precise sizing will depend upon the choice of device used.
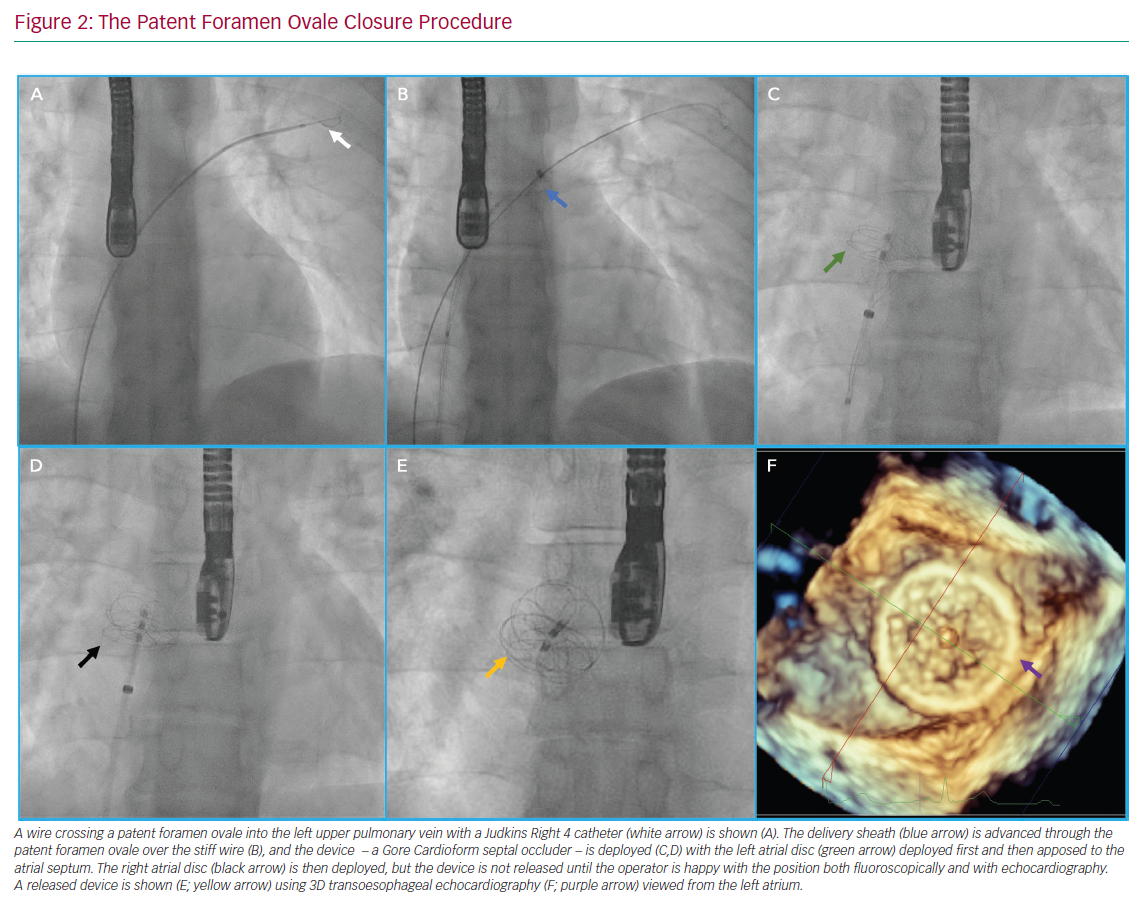
Once sizing is completed, an appropriate device (with delivery sheath) can be passed into the left atrium through the PFO. The left atrial disc is deployed, followed by the right disc. Ensuring that the delivery sheath remains de-aired and flushed throughout the procedure minimises the risk of air or thrombotic embolism. After the device is deployed, confirmation of the adequate position with echocardiography and fluoroscopy should be performed prior to device release. If the device is malpositioned after release, a large gooseneck snare can be used to recover the device. The steps involved in a PFO closure procedure are shown in Figure 2.
Evidence for antiplatelet therapy after device deployment remains incomplete. Device thrombosis remains a feared complication of PFO closure. In our practice, aspirin and clopidogrel are usually given for 6 months, but evidence for this is limited and practice varied markedly between trials. Earlier discontinuation of dual antiplatelet therapy was associated with an increased frequency of minor cerebrovascular events in a study level meta-analysis of PFO closure trials.66 Long-term observation studies have suggested this is a safe practice.33
Some operators preload patients with antiplatelets, but again, the evidence for this is uncertain. Single antiplatelet therapy, usually clopidogrel 75 mg daily, is continued indefinitely, as the device may take up to 5 years to endothelialise. The European Association for Percutaneous Cardiovascular Interventions consensus statement recommends this approach at present.66
Follow-up is important, but uncertainty remains about the appropriate timeframe. As most devices endothelialise over a period of approximately 6 months, then a repeat bubble study could be considered at that stage. Timing is of particular relevance where the PFO has been closed for occupational reasons, such as professional diving.
Closure Devices
A large number of devices with varying shape and size have been marketed. Many have received CE mark status in the EU. In the US, fewer devices have been approved by the Food and Drug Administration, due to the need for randomised evidence prior to approval.
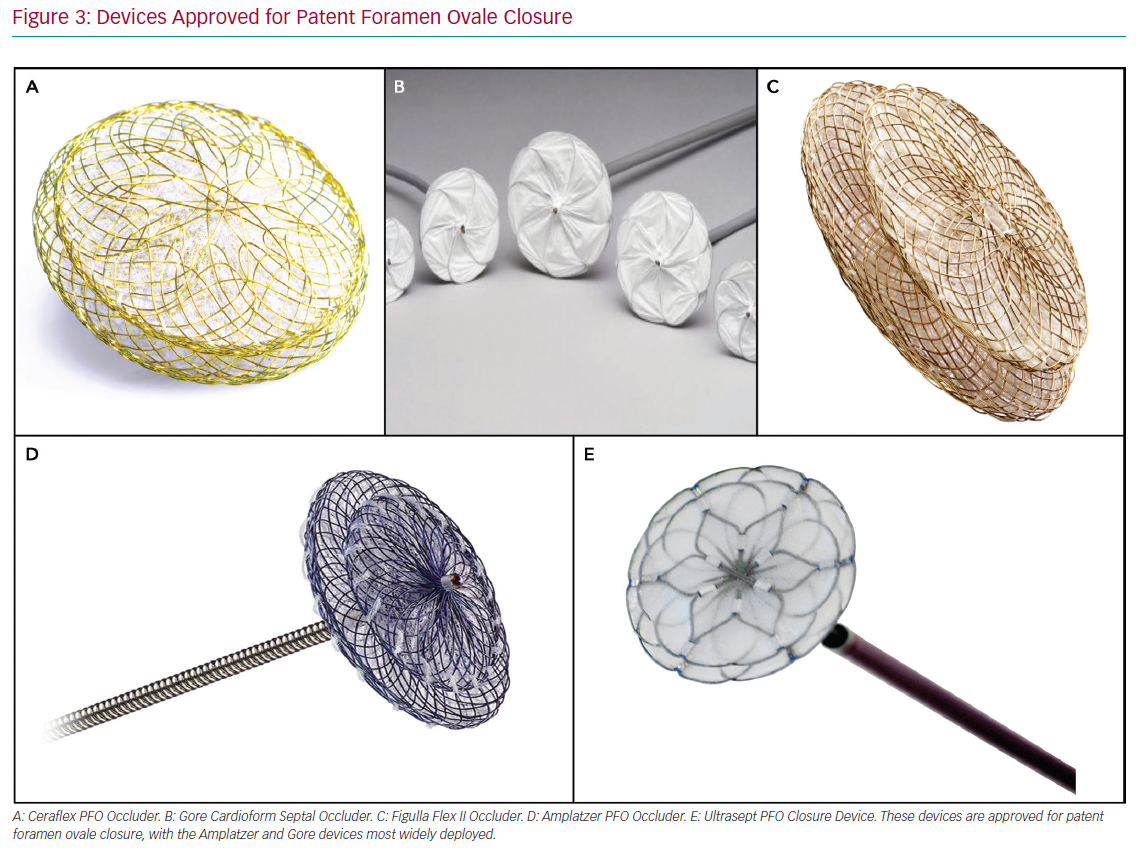
Most devices are of double-disc design, connected by a short waist. The Gore Septal Occluder (WL Gore and Associates) and the Amplatzer PFO Occluder (Abbott Vascular) are two of the more commonly used devices and are shown in Figure 3. The Gore Septal Occluder is constructed from five nitinol wires covered with expanded polytetrafluoroethylene.67 Early clinical experience has shown that it is a versatile device with easy deployment, high procedural success and low complication rates.68,69 The Amplatzer PFO Occluder is also a nitinol-based device. This device has been used most commonly in randomised clinical trials. The evidence base for its use is therefore very strong.21,22 There are numerous other commercially available devices, including the Occlutech PFO occluder (Occlutech International) and Ultrasept (Cardia), plus suture-based technologies, such as NobleStitch (HeartStitch).
Future Directions
There are a number of outstanding research questions regarding PFO closure that need to be answered. First, the optimal antiplatelet or anticoagulation regimen balancing the risk of recurrent stroke or embolism against the risk of bleeding needs to be established. Current guidance is based on consensus statements and the strategies adopted in the clinical trials mentioned earlier. Meta-analyses have not shown any clear additional benefit for anticoagulation when PFO is not closed after stroke.70 Further studies evaluating the benefit of anticoagulation and optimal duration of dual antiplatelet therapy would be welcome. Simplification of the procedure with the use of non-invasive echocardiography may be attractive, but is not recommended in consensus statements.64 A clinical trial to establish the safety and efficacy of a fluoroscopic approach with transthoracic echocardiography support is currently underway (NCT03828825).
Identification of a high risk of PFO-associated stroke prior to the first stroke remains the golden ticket. Some have published studies with scoring systems to identify high-risk PFO, but these have not identified patients prior to cryptogenic stroke, when the PFO is usually silent.71 Patients with inherited thrombophilia found to have PFO may be candidates for prophylactic PFO closure. Observational studies have suggested that those in this group who have a PFO closure have a reduced incidence of stroke or transient ischaemic attack.72 Randomised trials to assess whether this group would benefit are needed, but will be challenging to recruit, given the relatively small numbers of patients in this group.
A recent observational study of patients undergoing surgery found a significantly higher incidence of ischemic stroke over a 1-year period in those with PFO.73 This risk was mitigated for those receiving dual antiplatelet therapy or anticoagulation, or those who had undergone PFO closure. These observational data are hypothesis generating, but suggest that there may be a population that could be identified to benefit from upfront closure, but further well-designed clinical trials would be required to justify this against the procedural risk.
Furthermore, there are limited data to support differences in treatment by subgroup. A meta-analysis of trials reporting outcome by sex (RESPECT, REDUCE, CLOSURE 1) suggested that there was a significant reduction in men, and a non-significant numeral reduction in stroke for women. The majority of patients treated in these studies were men. Further work is required to identify whether there are meaningful differences in these groups. Similarly, differences between ethnic groups could also be examined.
Finally, expansion to other indications, particularly for migraine relief requires a better quality of evidence. The planned GORE CARDIOFORM Septal Occluder Migraine Clinical Study (RELIEF study) is a sham randomised controlled trial of PFO closure for migraine relief with recruitment due to start in 2020. A sham procedure is important to tease out the strong placebo effect associated with migraine studies (NCT04100135).
Conclusion
In this review, the main indications for PFO closure have been discussed (cryptogenic stroke, paradoxical systemic embolisation, platypnoea–orthodeoxia syndrome and decompression illness), together with the strengthening evidence for closure. The skills required for this procedure need to be learnt with the assistance of experienced interventional cardiologists who can proctor and advise those starting out with PFO closure. Attention to detail in the indication for the procedure, and minimising the risks to the patient during the closure are key to an effective PFO closure service.